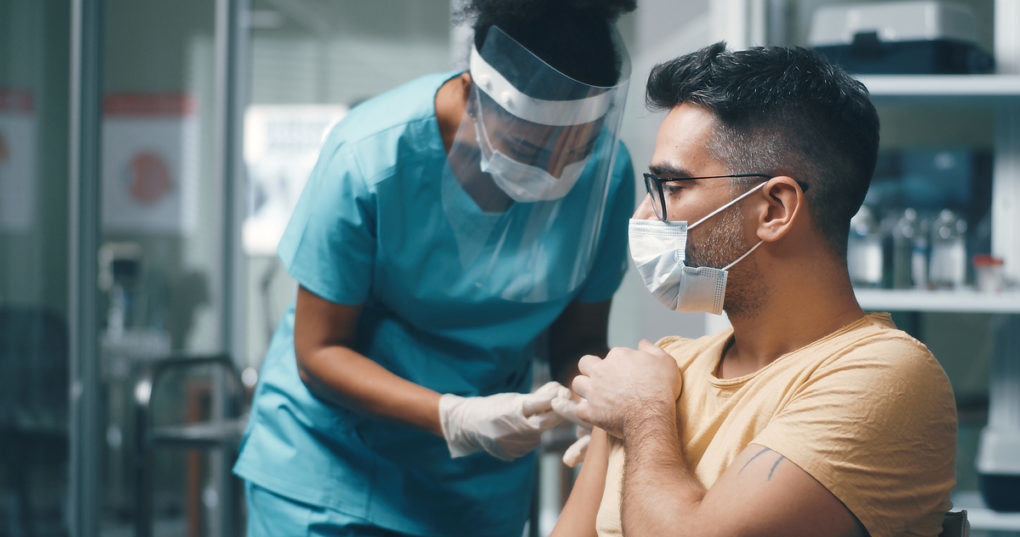
The rollout of the COVID-19 vaccine in the United States has been nothing short of spectacular. While the Biden administration’s goal was to administer 100 million vaccines during the new president’s first 100 days in office, that goal significantly underestimated production. The country is now on track to administer nearly 200 million doses in the first 100 days.
Entering phase two of the vaccine rollout supply is outpacing demand across the U.S. While we should send excess supplies to countries suffering—as the Biden administration recently pledged to do—public health officials and policymakers must combat vaccine hesitancy and anti-vaccination sentiments, two historically strong forces in the country. Without most of the country’s population vaccinated, we cannot reach herd immunity. For those of us who cannot receive vaccines due to age or health reasons, the risk of serious COVID-19 cases, complications, and death remains. The question we must answer now is how the U.S. and other countries can convince the 37% (in the U.S.) of individuals with some degree of vaccine hesitancy to get vaccinated.
A Historical Hesitancy
Vaccine hesitancy, or the personal reluctance or refusal to be vaccinated or allow one’s children to be vaccinated, is a public health issue as old as the first vaccines. Such an issue is not unique to the United States. In fact, one of the first anti-vaccination movements occurred in Stockholm in the 1870s, where a smallpox vaccination campaign failed in urban Stockholm due to concerns about efficacy, individual rights, and religious prohibition of vaccines. The idea that vaccines were a method to defy “God’s will” led to a vaccination rate of 40%, a considerable decline from the country-wide average of 90%. This hesitancy to receive vaccinations saw increased death rates within the nation’s capital.
While there are numerous reasons that a person can become vaccine hesitant, the motivations can be broadly classified into three buckets: individual liberty, religious liberty, and distrust of institutions. As a country, our founding principles enshrine both individual and religious liberty, while our medical system’s history of testing on the poor and people of color, such as the Tuskegee Study of 1972, contributes to a distrust of physicians and pharmaceutical companies among older and more diverse populations.
Informational Overload
This unique combination of factors in the U.S. has halted conversations between those in favor of and those against vaccines. Both sides are “telling” the other side what is right, and policymakers are failing to “show” the benefits that come from vaccination. Policymakers and public health officials put together dossiers of information, TV commercials, radio, print ads, etc., that share vaccine benefits, outline potential side effects, and dispel the common myths around the vaccine. This communication strategy is called the Information Deficit Model, or the assumption that vaccine-hesitant people simply do not have enough information to make the choice to get vaccinated. With this line of thinking, the right information can result in a conversion.
Unfortunately, vaccine-hesitant persons often have access to all the right information, and they refuse to trust. Distrust may be connected to the source, often government or institutional medicine. Many of those who refuse vaccines are equipped with information that contradicts pro-vaccine information; they get it from more-trusted networks, like social media-readily available anti-vax videos. When governments provide more information to push a change of heart, it’s often vaccine-hesitant people who “dig in” and become even more disinclined to receive the vaccine.
The Power of Imagery
If more information won’t convince the vaccine-hesitant population to change their behavior, what can be done? On both an interpersonal and collective level, we must show rather than tell the benefits of being vaccinated.
What does show mean on an interpersonal level? It’s relatively simple. Once you’re vaccinated, tell your friends, family, and colleagues. Post on social media, go to work, and continue interacting with others—show them that nothing is wrong with you now that you’re vaccinated. Recent polling shows that simply knowing someone who is vaccinated decreases one’s likelihood of being vaccine hesitant. If you’re reading this and are vaccinated or are soon to be vaccinated, you can help solve the problem just by communicating with others in your social network and “showing” them there’s nothing to fear.
But the country should go further if needed. To “show” vaccine-hesitant members of the population the benefits of being vaccinated, we should incentivize it on a policy level.
Putting It on Paper
There’s been much ado regarding the topic of vaccine passports—devices, apps, or paperwork that shows one’s vaccination status and allows them access to specific events or services. Many conservative states are banning such documents and technology. The federal government does, however, have the authority to override these bans through commerce clause powers in the U.S. Constitution.
Both state and federal government should take action that implements benefits for fully vaccinated people. For example, in Illinois, outdoor events are limited to 100 persons; however, a vaccinated person does not count towards an event’s total number of attendees. In theory, an event could proceed at full capacity if everyone is vaccinated. The federal government should create a policy on these types of interventions and establish a methodology for tracking vaccine passports to avoid fraud or misuse.
Blasting Them with Benefits
Access to previously restricted activities may not be enough. Should vaccine hesitancy continue to inhibit herd immunity after such passport-type policies are launched, the government should further incentivize vaccination. Positive ways to encourage vaccination may include a tax credit for being fully vaccinated or a special benefit program.
The government can “show” unvaccinated people that they are missing out on a return to normalcy by providing visible benefits. Vaccinated persons enjoying these benefits will likely post on social media, and major media outlets will pick up stories and pictures that demonstrate a return to normal. For a vaccine-hesitant person, a desire for life, as usual, may be the final push needed to get a vaccine themselves.
While very few countries have reached the point where vaccine supply has outpaced demand, it is on the horizon for some. The U.S. has an opportunity to lead the world forward in developing strategies to combat vaccine hesitancy. Let’s work together to show the vaccine-hesitant people among us that there is nothing to fear and much to gain by getting the jab.